TL;DR — Patient Retention Strategies
- Retaining an existing patient costs 5–7× less than acquiring a new one — retention is the highest-ROI growth lever in dentistry.
- The industry benchmark for active patient retention is 85%+; most practices sit at 60–70% without realizing it.
- Systematic recall, proactive scheduling, and personalized communication each independently improve retention by 10–20 percentage points.
- Dental anxiety affects 36% of patients and is the most common hidden reason for appointment gaps — addressing it directly reduces attrition.
- A structured loyalty and referral program converts retained patients into an active referral pipeline.
The most effective dental practice growth strategy isn’t marketing — it’s keeping the patients you already have. ADA Health Policy Institute data consistently shows that replacing a lost patient costs between $200 and $400 in marketing and administrative overhead, while a retained patient generates predictable recurring revenue at near-zero acquisition cost. Yet most practices invest heavily in new-patient campaigns while doing little to systematically retain the active base they’ve spent years building.
This guide outlines evidence-backed dental patient retention strategies your practice can implement immediately: from the scheduling systems that prevent patients from drifting away to the communication frameworks that make patients feel known, not processed. These strategies are part of the broader framework covered in our guide to effective growth strategies for dental practices.
What Is the True Cost of Patient Attrition?
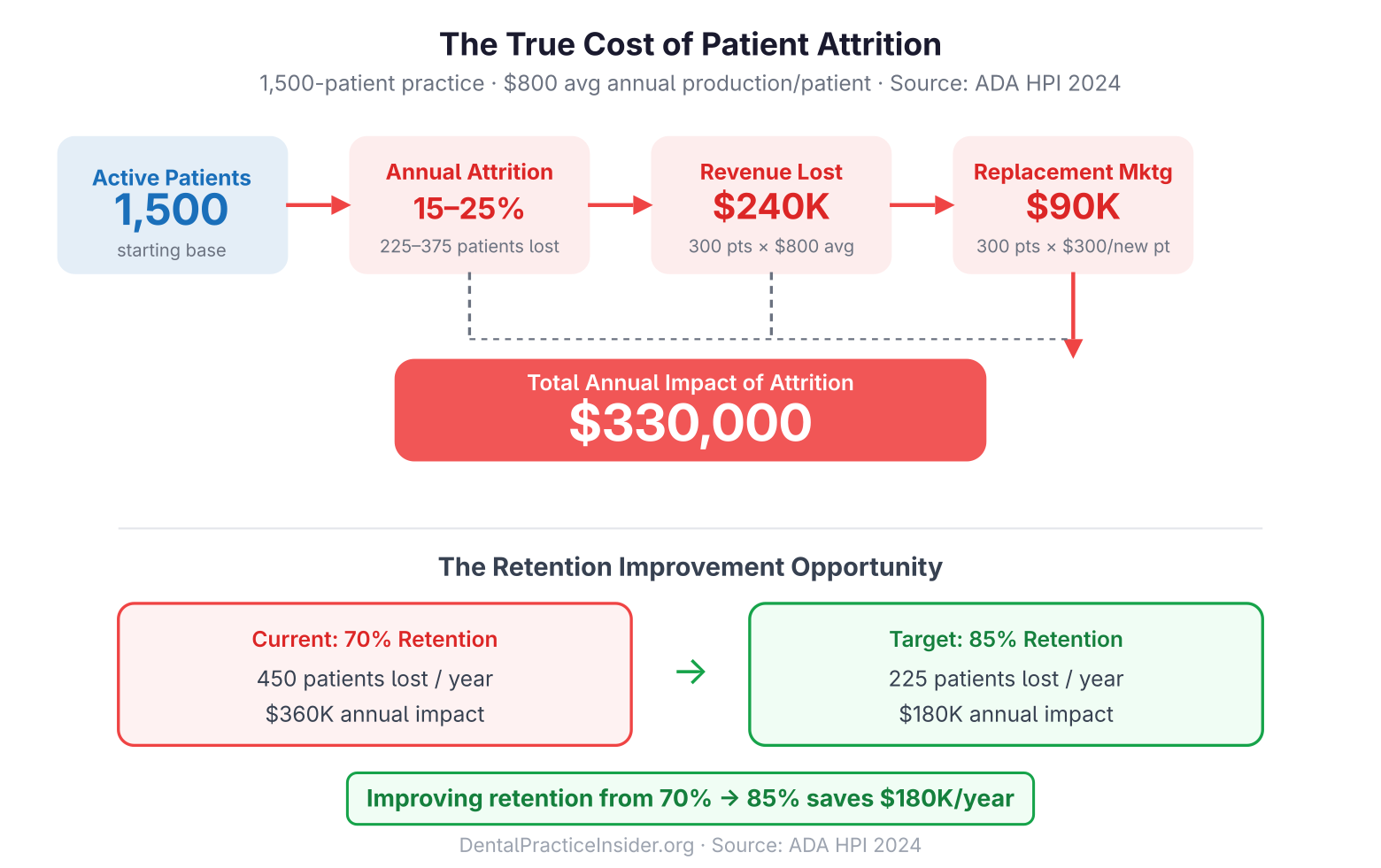
Patient attrition is the silent drain on practice revenue that rarely shows up on a P&L until it becomes a serious problem. The ADA Health Policy Institute estimates that the average general practice loses 15–25% of its active patient base each year through a combination of relocation, insurance changes, unaddressed dissatisfaction, and simple neglect — meaning a practice with 1,500 active patients may be losing 225–375 patients annually without a formal retention system.
For related reading, see our guide on modern dental practice management.
The financial math is straightforward. If your average patient generates $800 per year in production, losing 300 patients represents $240,000 in annualized revenue that must be replaced through new-patient acquisition before the practice can grow at all. At a cost-per-new-patient of $300, replacing those 300 patients costs $90,000 in marketing alone — before accounting for staff time, onboarding, and the revenue gap during the replacement period.
Viewed this way, improving your retention rate by 10 percentage points — from 70% to 80% on a 1,500-patient base — prevents the loss of 150 patients, saving $120,000 in annual production and $45,000 in replacement marketing. No marketing campaign delivers that return.
How Do You Measure Patient Retention in a Dental Practice?
Before improving retention, you need to measure it accurately. Most practice management software tracks this differently, but the core calculation is consistent:
Retention Rate = (Patients who completed a recall visit in the past 18 months ÷ Total patients seen in the prior 18-month period) × 100
An 18-month window is standard because it captures patients on both 6-month and 12-month recall cycles. A rate above 85% is considered healthy by dental industry benchmarks. A rate below 70% indicates a structural problem — typically in scheduling, communication, or patient experience — that no amount of new-patient marketing can fix sustainably.
For related reading, see our guide on dental practice economics.
Secondary metrics to track alongside retention rate include:
- Reappointment rate at checkout: What percentage of patients leave with their next appointment scheduled? Aim for 85%+ pre-scheduled at checkout.
- Recall compliance rate: Of patients due for recall in a given month, what percentage actually complete it? Benchmark is 80%.
- Lapsed patient count: Patients who haven’t been seen in 18+ months but are still in your system. This number should shrink each quarter with an active reactivation program.
What Scheduling Systems Prevent Patients From Drifting Away?
The single most effective retention tool in dentistry is pre-scheduling the next appointment before the patient leaves the office. A 2022 study published in the Journal of Dental Education found that patients who leave a visit with a confirmed future appointment attend that appointment at an 83% rate, compared to a 54% rate for patients who are contacted later by phone or text to schedule (ADA, 2022).
Effective scheduling systems for patient retention include:
Pre-Scheduling at Checkout
Train every front desk team member to present the next appointment as a given, not an option: “Your next cleaning is scheduled for October 14th at 2pm — does that time work for you?” is dramatically more effective than “Would you like to schedule your next appointment?” The former requires a patient to opt out; the latter requires them to opt in.
Automated Recall Sequences
Implement a multi-touch recall sequence for patients without a future appointment: an email or text at the 5-month mark, a follow-up at 6 months, and a personal phone call at 7 months from a team member they know by name. Software platforms such as Weave, Lighthouse 360, and Solutionreach automate the first two touches while flagging unresponsive patients for personal outreach.
Same-Day Scheduling for Urgent Needs
Reserve 2–3 same-day slots daily for urgent care. Patients who call with tooth pain and hear “we can see you today” become loyal advocates; patients who are told to wait two weeks often become someone else’s patient and don’t return.
How Does Patient Communication Drive Retention?
Patients who feel known — not just processed — are far less likely to switch providers. Communication is the primary mechanism for creating that feeling at scale. The goal is to make each touchpoint feel personal even when it’s systematized.
Personalized Appointment Reminders
Generic reminders (“You have an appointment on Tuesday”) are table stakes. High-retention practices send reminders that reference the patient’s specific situation: “Hi Sarah — just a reminder that your 6-month cleaning is Tuesday at 10am. Dr. Johnson will also check on the tooth sensitivity you mentioned in January.” This requires that your clinical notes capture patient concerns and that your recall software or team can surface them before outreach.
Post-Treatment Follow-Up Calls
A brief call or text the evening after any procedure longer than a cleaning communicates genuine care. The message doesn’t need to be elaborate — “Just checking to make sure you’re comfortable after today’s work” accomplishes the goal. According to a 2023 patient experience report by Press Ganey, patients who receive post-procedure outreach are 40% more likely to rate their experience as excellent and 2× as likely to refer a friend or family member (Press Ganey, 2023).
Birthday and Milestone Acknowledgments
Automated birthday messages, when they feel personal rather than robotic, create low-cost touchpoints between appointments. A brief, warm message — not a promotional offer — is the appropriate format. Practices that send promotional coupons on birthdays consistently score lower on patient experience surveys than those that send simple personal acknowledgments.
What Role Does Dental Anxiety Play in Patient Attrition?
Anxiety is the most under-addressed driver of patient loss in dentistry. Research published in the Journal of Dental Research estimates that dental anxiety affects 36% of the general population, with 12% experiencing extreme fear (Armfield & Heaton, 2013). These patients don’t call to cancel — they simply stop scheduling. They appear as lapsed patients in your system with no obvious reason for leaving.
Retention strategies that specifically address dental anxiety include:
- Screening at intake: Add a single question to your new patient intake form — “On a scale of 1–10, how anxious do you feel about dental visits?” — and flag high scorers for additional communication and accommodation.
- Communicate sedation options proactively: Anxious patients often don’t ask about sedation because they don’t know it’s available. A brief mention during the first visit (“Many of our patients find nitrous very helpful — let me know if you’d like to try it”) removes the barrier.
- Establish a “stop signal”: Giving patients a hand signal or word to pause treatment instantly eliminates the helplessness that drives avoidance behavior. This costs nothing and dramatically reduces no-show rates among anxious patients.
For a deeper exploration of how communication builds patient confidence and reduces attrition, see our article on how to improve patient satisfaction in your dental practice.
How Can Loyalty and Referral Programs Reinforce Retention?
Well-designed loyalty programs serve two functions: they reward behavior patients were already likely to engage in (keeping appointments, accepting treatment), and they create a concrete reason for patients to choose your practice over a competitor when they’re on the fence. The key is keeping the structure simple — complicated point systems create administrative overhead and patient confusion.
Membership Plans as a Retention Tool
In-house dental membership plans — typically $25–$40/month for adults — offer covered cleanings and discounts on other services in exchange for a recurring subscription. For uninsured patients, membership plans provide genuine value. For practices, they guarantee a revenue stream and dramatically improve retention among a population that would otherwise skip appointments due to cost concerns. Practices that offer membership plans consistently report higher recall compliance rates among enrolled members than among insured patients.
Structured Referral Programs
Referral programs work best when the incentive is modest and the ask is explicit. Training front desk staff to say “We love working with patients like you — if you have friends or family who need a dentist, we’d be grateful for the referral” costs nothing. Adding a small gesture — a handwritten thank-you note plus a $25 credit on their account — formalizes the appreciation without creating legal or ethical issues related to fee-splitting.
How Does Team Training Affect Patient Retention?
Patient retention is ultimately a team-level outcome. Every patient interaction — from the initial phone call to checkout — either builds or erodes the relationship. Practices with high turnover or inconsistent front desk behavior show measurably lower retention rates because patients lose continuity and the sense of being known.
High-retention practices invest in:
- Scripted language for common friction points: How team members handle insurance disputes, scheduling conflicts, and cost conversations directly determines whether patients feel respected or processed. Scripting the highest-stakes interactions ensures consistency.
- Regular team training on patient experience: Quarterly training sessions focused on communication, empathy, and handling complaints keep standards high. This doesn’t require expensive external consultants — role-playing difficult conversations within the team is highly effective.
- Recognizing team members who drive retention: Track recall compliance, reappointment rates, and patient satisfaction scores by team member. Recognize and reward top performers publicly.
Operational efficiency and team performance are explored in depth in our guide to dental practice operations and efficiency strategies.
What Technology Investments Best Support Patient Retention?
Technology should automate the systematizable parts of retention — reminders, recalls, reviews — while freeing your team to invest time in the human interactions that technology can’t replicate.
The highest-ROI technology investments for retention are:
- Patient communication platforms (Weave, Lighthouse 360, Solutionreach): Two-way texting, automated recall, online scheduling, and review requests in a single system. Cost: $300–$600/month. Return: typically 10–15 additional retained patients per month within 90 days.
- Patient portals: Online bill pay, treatment plan review, and form completion reduce friction at every touchpoint. Patients who use a portal visit more consistently than those who don’t.
- Reputation management: Automated review requests sent within 2 hours of a positive appointment build the online reputation that makes new patient acquisition easier and confirms existing patients’ decision to stay.
For broader context on how patient relationships connect to practice growth, see our pillar guide on building patient trust and relationships (Cluster C).
What Is a Realistic Timeline for Improving Patient Retention?
Retention improvements follow a predictable curve. The first 90 days are primarily structural — implementing pre-scheduling at checkout, activating an automated recall system, and training the team on communication language. These changes show up in reappointment rates within the first month.
Months 3–6 show measurable improvement in recall compliance as the automated sequences reach the full patient base. Lapsed patient reactivation campaigns run concurrently, typically recovering 5–15% of patients who haven’t been seen in 12–24 months.
By month 12, retention rate should improve by 10–15 percentage points if all systems are implemented consistently. This is when the compounding effect begins — retained patients refer more, accept more treatment, and require less administrative overhead per visit than new patients.
Summary: Building a Retention-First Practice
Dental patient retention is not a single tactic — it’s a system that includes scheduling, communication, clinical experience, team culture, and technology. The practices that grow most consistently are those that treat retention as a core business discipline rather than an afterthought to marketing.
Start with the two highest-use actions: implement pre-scheduling at checkout today, and activate an automated recall sequence this week. Those two changes alone will improve your retention rate within 90 days. Build from there systematically, and the compounding effect will make every other growth investment more efficient.
Last Updated: March 2026
Sources
- American Dental Association Health Policy Institute. Patient Retention and Recall Benchmarks. ADA, 2022.
- Armfield, J.M. & Heaton, L.J. “Management of fear and anxiety in the dental clinic: a review.” Australian Dental Journal, 2013.
- Press Ganey. 2023 Consumer Experience Trends in Healthcare. Press Ganey Associates, 2023.
For more resources on this topic, see our complete guide to patient trust and experience.



