What Is Dental Insurance Credentialing?
Credentialing is the process by which an insurance plan verifies your qualifications, licensure, and background before adding you to their network as a participating provider. Until you’re credentialed and contracted, you cannot bill that plan as an in-network provider—even if the patient has coverage and you’re treating them.
For related reading, see our guide on creating a dental membership plan.
For related reading, see our guide on negotiating better dental insurance rates.
For related reading, see our guide on managing PPO plan risks.
For related reading, see our guide on PPO transition success stories.
Two distinct processes often get confused:
- Credentialing: The insurance company verifies your credentials (degree, license, malpractice history, DEA registration)
- Contracting: You and the plan agree to fee schedules and terms of participation
Both must be complete before you can submit in-network claims. Contracting sometimes occurs simultaneously with credentialing; other plans credential first and contract separately.
Why Does Credentialing Take So Long?
90-120 days feels unreasonable. Here’s why it happens:
- Credentialing committees at large insurers (Delta Dental, MetLife, Cigna, Aetna) meet on fixed schedules—monthly or quarterly—so a missed cycle adds 30–90 days
- Primary source verification requires contacting dental schools, licensing boards, and malpractice carriers directly—these sources have their own response timelines
- Incomplete applications are returned, restarting the clock
- Plan-specific application formats mean no standardization across 20+ plans you may want to join
The CAQH ProView database (Council for Affordable Quality Healthcare) reduces some redundancy by centralizing provider data that multiple plans can access. Completing your CAQH profile is often step one.
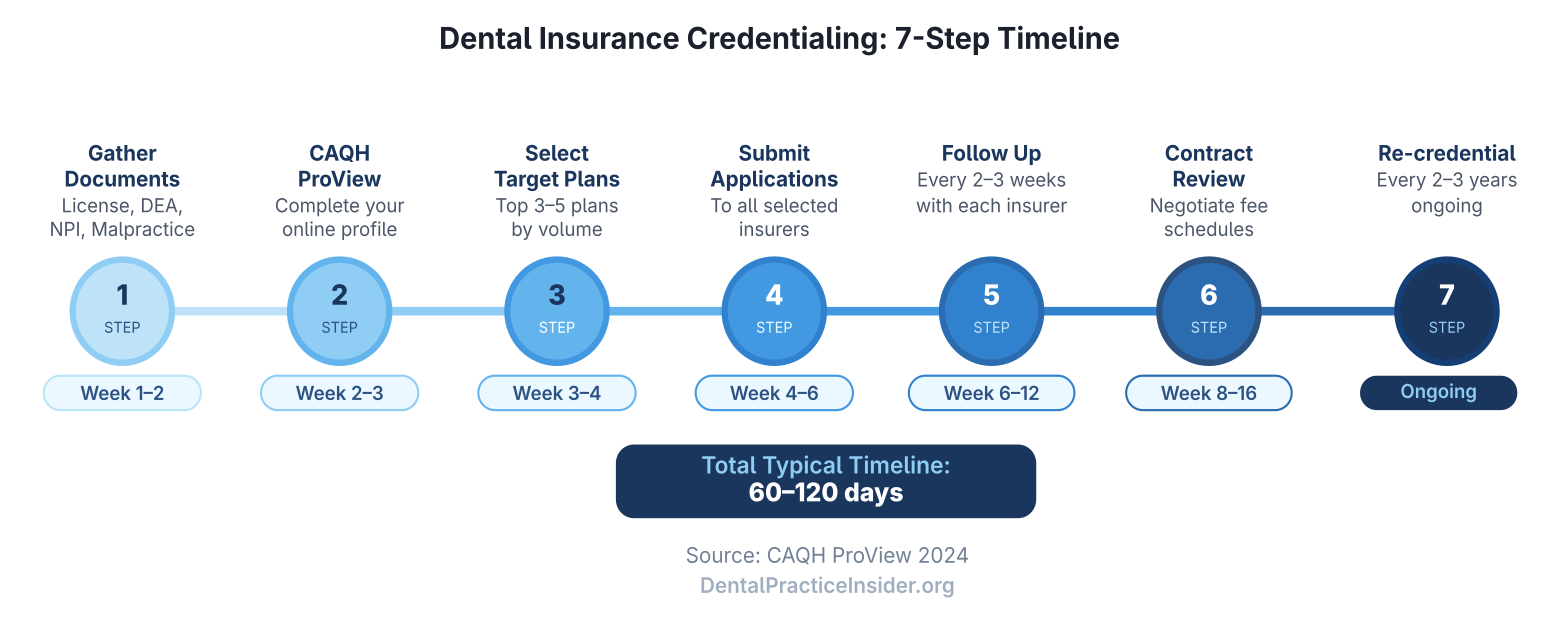
Step-by-Step: How to Get Credentialed with Dental Insurance Plans
Step 1: Gather Your Credentials Documents
Have these ready before submitting a single application:
- Dental school diploma and transcripts
- Current state dental license (all states where you practice)
- DEA registration certificate
- National Provider Identifier (NPI) — Type 1 (individual) and Type 2 (practice entity)
- Malpractice insurance certificate with carrier name, policy number, and coverage limits
- CAQH ProView username and completed profile
- CV / work history for the past 5–10 years (no gaps)
- Specialty board certification certificate (if applicable)
- Hospital or surgical center privileges documentation (if applicable)
- Practice EIN (Tax ID) and business entity documents
- Signed W-9
- Voided check for electronic funds transfer (EFT) setup
Step 2: Complete and Maintain Your CAQH ProView Profile
CAQH ProView (caqh.org) is used by most major commercial insurers as their primary credentialing data source. Complete every field. Upload all documents. Re-attest your profile every 120 days—if your profile lapses, credentialing applications using it stall.
Step 3: Identify Which Plans to Apply For
Don’t credential with every plan by default. Analyze your target patient population:
- Which plans do your neighbors’ employers offer? (Call HR departments or check employer websites)
- What plans do prospective patients ask about most when calling?
- Which plans have reasonable fee schedules in your zip code? (Request fee schedules before applying—plans must provide them upon request)
Start with the 3–5 highest-volume plans in your market. Delta Dental, MetLife, Cigna, United Concordia, and Aetna cover the majority of commercially insured dental patients in most U.S. markets.
Step 4: Submit Applications
Each plan has its own application process. Some use online portals; others require paper applications. Call the provider relations department for each plan to get current instructions and the direct contact for your application.
Submit all applications simultaneously—don’t wait for one approval before starting the next. Each runs its own parallel timeline.
Step 5: Follow Up Proactively
Call or email provider relations every 2–3 weeks after submission. Ask for:
- Confirmation that the application was received
- Whether any documents are missing or need updating
- Your estimated effective date
Document every contact: date, representative name, and what was discussed. If there’s a dispute later about your effective date, this log is your evidence.
Step 6: Review and Sign Your Provider Contract
Before signing, review:
- Fee schedule for your top 20 most-billed CDT codes
- Termination clauses (how much notice is required to leave the plan?)
- Clean claim submission timeframes
- Coordination of benefits (COB) policies
- Whether the contract allows “fee-for-service” billing to uninsured patients or restricts your non-plan fees
Step 7: Set Up Re-Credentialing Reminders
Most plans require re-credentialing every 2–3 years. Missing re-credentialing deadlines can result in termination from the plan and loss of in-network status. Set calendar reminders 90 days before each plan’s re-credentialing window opens.
What Are the Most Common Credentialing Mistakes?
- Starting too late (6-month minimum lead time before you need to bill)
- Submitting incomplete applications (read every field carefully; plans reject incomplete apps without calling you)
- Letting your CAQH profile lapse (re-attest every 120 days)
- Not tracking application status (no follow-up = applications lost in the queue)
- Signing contracts without reviewing fee schedules (you may be locking in low fees for 2–3 years)
- Forgetting to add new providers when an associate joins (their applications run the same 60–120 day timeline)
Should You Use a Credentialing Service?
Credentialing services charge $100–$300 per application plus ongoing maintenance fees. For a startup practice applying to 8–12 plans simultaneously, that’s $800–$3,600 in service fees—often worth it when your time is better spent treating patients and building the practice.
Well-regarded dental credentialing services include Dental Credentialing Associates, Apex EDI, and CredentialStream (part of symplr). Verify that any service you use has direct relationships with the plans you’re applying to and references from practices in your state.
For a strategic view on managing insurance dependency over the long term, see our guide on reducing insurance dependency in dental practices.
Frequently Asked Questions
Can I see patients before credentialing is complete?
Yes, as an out-of-network provider. Patients with out-of-network benefits may still receive partial reimbursement. Some plans offer retroactive claims processing once credentialing is approved—ask each plan specifically about this option before assuming it applies.
How long does Delta Dental credentialing take?
Delta Dental typically takes 60–90 days. Processing times vary by state affiliate—Delta Dental operates through state-based chapters, each with independent credentialing processes. Apply to the state chapter where your practice is located.
What is a credentialing effective date?
Your effective date is the date your in-network participation begins. You can only bill in-network claims for services rendered on or after this date. Some plans backdate the effective date to your application date if approved within a certain window—ask about this when following up.
Do I need to credential with Medicaid separately?
Yes. Medicaid credentialing is handled by your state’s Medicaid agency, not the commercial insurers. Timelines vary widely by state (30–180 days). Some states use managed care organizations (MCOs) that have their own credentialing processes layered on top of state enrollment. Start early.
What happens if a plan terminates my participation?
Plans can terminate participation with 30–90 days notice (varies by contract). You have the right to appeal in most cases. Upon termination, you must notify patients of your change in network status and continue care for a transition period (typically 30–90 days for active treatment cases). Review your contract’s termination terms before signing—look for “without cause” termination clauses and required notice periods.
For more resources on this topic, see our complete guide to insurance independence strategies.



