TL;DR — Dental Patient Satisfaction
- 72% of dental patients cite “feeling listened to” as the primary driver of satisfaction — clinical outcome is secondary (ADA, 2023).
- The single highest-use satisfaction improvement is scripting the appointment handoff — how patients feel when they leave determines whether they return and refer.
- Addressing dental anxiety proactively doubles case acceptance and near-eliminates repeat no-shows from anxious patients.
- Post-procedure follow-up calls increase the probability of a 5-star review by 2× and referral likelihood by 40%.
- Patient satisfaction and patient retention are the same metric measured at different time horizons — improving one improves the other.
Patient satisfaction in a dental practice is determined less by clinical excellence than most dentists expect, and more by how patients are made to feel at every non-clinical touchpoint. Research consistently shows that patients are poor judges of clinical quality — they cannot accurately evaluate whether a crown margin is perfect or whether a composite restoration will last 10 years. What they can evaluate precisely is whether they felt heard, whether the team treated them as a person rather than an appointment, and whether the experience was worth the time and cost.
For related reading, see our guide on reducing patient no-shows.
This guide translates that insight into specific, actionable strategies that raise patient satisfaction scores, improve online reviews, and build the kind of patient loyalty that generates referrals without a marketing budget. These strategies form the operational layer of the broader framework covered in our pillar guide on building patient trust and relationships.
For related reading, see our guide on dental practice marketing strategies.
What Do Dental Patients Actually Want From Their Experience?
A 2023 American Dental Association patient experience survey found that when asked what factors most influenced their overall satisfaction with a dental visit, patients ranked the following in order:
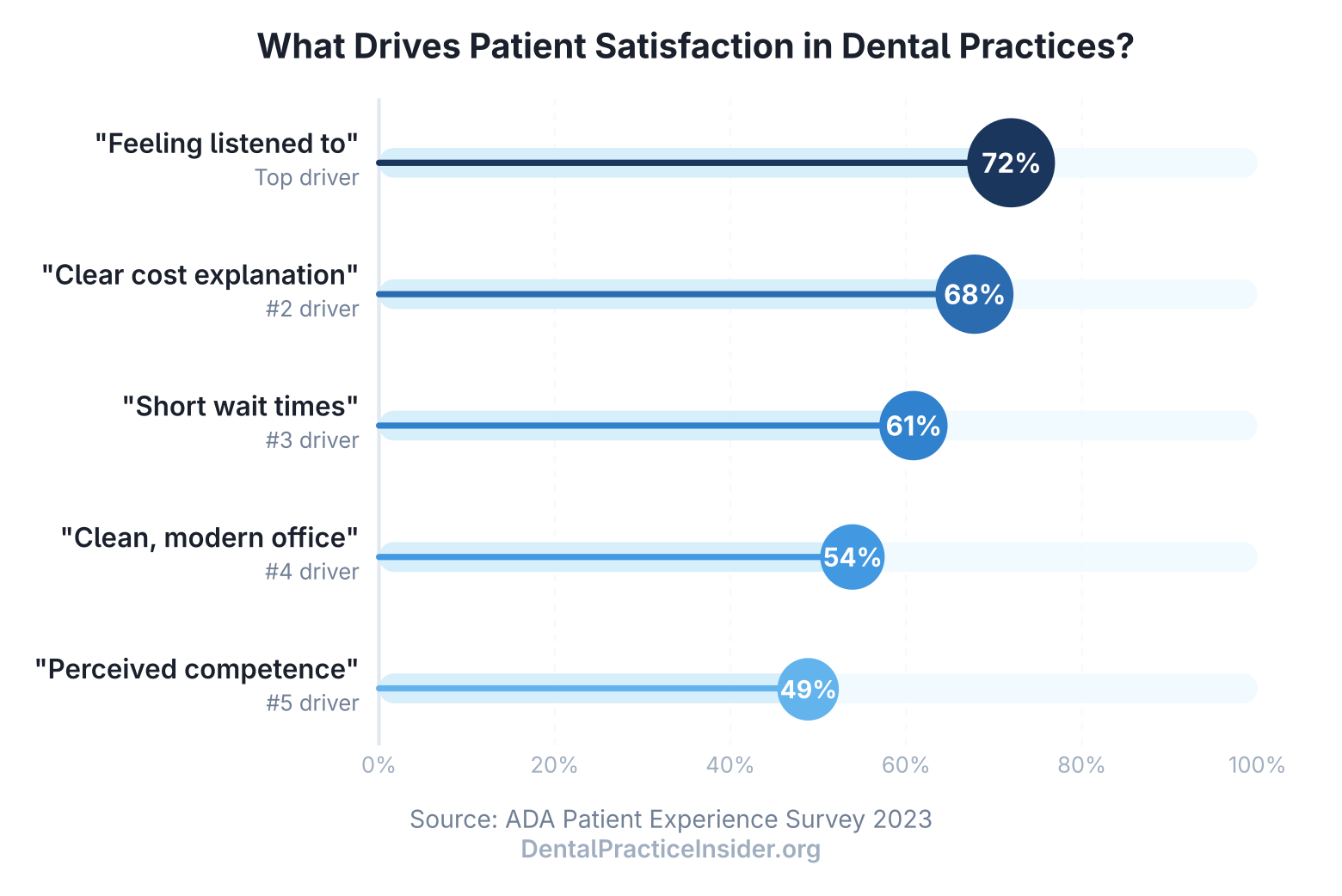
- Feeling listened to by the dentist and team (72%)
- Clear explanation of treatment and costs before proceeding (68%)
- Short wait times (61%)
- A clean, modern office environment (54%)
- Perceived clinical competence (49%)
The clinical excellence that dentists understandably prioritize ranks fifth. This isn’t a reason to deprioritize clinical quality — it’s a reason to recognize that clinical quality is necessary but not sufficient, and that the other four factors represent the satisfaction gap where most practices can improve most quickly (ADA, 2023).
How Does Communication Drive Dental Patient Satisfaction?
Communication is the primary mechanism through which patients form their experience of a dental visit. A technically excellent procedure delivered with poor communication produces lower satisfaction than an average procedure delivered with excellent communication. This is not intuition — it’s a pattern documented consistently in healthcare satisfaction research.
The First Phone Call
Patient satisfaction begins before the first visit. The tone, response time, and information quality of the initial phone call or online inquiry response sets expectations that are difficult to exceed if they start poorly. Practices with high satisfaction scores typically answer calls within 3 rings, use the caller’s name at least twice in the conversation, confirm next steps explicitly, and end with a statement that makes the patient feel expected and welcomed — “We’re looking forward to meeting you, Sarah.”
The Chair-Side Experience
The clinical appointment is the highest-stakes communication window. Three practices that consistently appear in high-satisfaction dental practices:
- Narrate before doing: Briefly describing what you’re about to do before doing it — “I’m going to place some numbing gel, you’ll feel a cool sensation” — reduces anxiety and eliminates the element of surprise that drives discomfort perception upward.
- Check in during the procedure: A mid-procedure hand signal or pause (“How are you doing? Any discomfort?”) gives patients a sense of control and communicates care. Patients who feel in control during dental procedures report significantly lower pain perception than those who don’t.
- Close with a summary: Before the patient transitions to checkout, provide a 30-second summary of what was done, what to watch for, and what comes next. Patients who receive this summary are significantly more likely to follow post-care instructions and less likely to call with anxious follow-up questions.
The Checkout Experience
Checkout is the last impression of the visit and the moment most patients decide whether they’ll schedule their next appointment. A checkout experience that feels rushed, transactional, or focused on payment processing leaves patients with a negative final impression that colors the entire visit. High-satisfaction practices train checkout staff to acknowledge the patient’s experience before discussing payment — “How did everything go today?” — and to present the next appointment as an expected next step, not an optional upsell.
How Does Addressing Dental Anxiety Improve Patient Satisfaction?
Dental anxiety is not a fringe issue — it affects approximately 36% of adults to some degree, with 12% experiencing dental phobia severe enough to avoid necessary care (Armfield & Heaton, 2013). For practices with any significant proportion of anxious patients, anxiety management is a direct driver of satisfaction, retention, case acceptance, and even revenue — because anxious patients who feel safe complete more treatment than those who avoid care.
Identifying Anxious Patients Early
Add a single question to your new patient intake form: “How comfortable do you feel about dental visits, on a scale of 1–10?” Patients who score 5 or below should be flagged for additional communication before and during the visit. This flag alerts the clinical team to take specific steps — offering a meet-and-greet before the procedure begins, allowing extra time for questions, confirming sedation options — that can transform the experience.
Sedation Options and Comfort Measures
Many anxious patients don’t ask about nitrous oxide or oral sedation because they don’t know it’s available or are embarrassed to ask. Proactively mentioning comfort options — “We offer nitrous for patients who prefer it; many people find it very helpful” — removes the barrier and gives patients a sense of control over their experience. Comfort measures that require no technology — weighted blankets, noise-canceling headphones, a clear stop signal — also measurably reduce anxiety and improve post-visit satisfaction ratings.
What Physical Environment Factors Drive Patient Satisfaction?
Patients form immediate, subconscious judgments about a practice based on sensory inputs they may not consciously register: ambient noise levels, the smell of the waiting area, the cleanliness and modernity of visible equipment, the temperature of the room. These environmental signals communicate competence and care before a word is spoken.
The highest-impact environmental improvements, ranked by effect on patient satisfaction scores:
- Waiting time: Patients who wait more than 10 minutes past their scheduled appointment time without acknowledgment report significantly lower satisfaction. The solution isn’t eliminating delays — delays happen in all clinical environments — it’s proactive communication when delays occur. “I wanted to let you know Dr. Chen is running about 12 minutes behind — can I get you a coffee while you wait?” converts a frustrating wait into a trust-building moment.
- Cleanliness and visible sterilization: Post-pandemic patients notice and evaluate visible hygiene practices. Clean, uncluttered operatories with visible autoclave equipment signal competence in ways that patients can perceive and articulate.
- Natural light and noise management: Operatories with natural light and managed ambient noise (quiet background music, not televisions at high volume) consistently outperform sensory-overloaded environments on patient comfort ratings.
How Should Practices Handle Patient Complaints to Preserve Satisfaction?
How a practice handles complaints is often more important to long-term satisfaction than whether the complaint arose in the first place. Research across healthcare settings consistently finds that patients whose complaints are addressed promptly and empathetically report higher subsequent satisfaction scores than patients who had no complaint — a phenomenon researchers call the “service recovery paradox.”
The effective complaint response protocol has four steps:
- Acknowledge without defending: “I’m sorry that happened — that’s not the experience we want you to have.”
- Ask questions to understand the specific issue: Don’t assume; ask what specifically went wrong from the patient’s perspective.
- Resolve within 24 hours: Even if the resolution is complex, communicate within 24 hours that you’ve heard the complaint and are working on it. Silence after a complaint is the primary driver of negative reviews.
- Follow up after resolution: A brief call or text confirming that the issue was addressed and asking whether the patient is satisfied with the outcome closes the loop and signals genuine care.
How Do Online Reviews Reflect and Reinforce Patient Satisfaction?
Online reviews are the externally visible output of your patient satisfaction system. A practice averaging 4.8 stars across 200+ Google reviews is signaling to prospective patients that the experience is consistently high-quality. A practice with 4.2 stars and recent negative reviews is signaling uncertainty.
The highest-converting review request moment is within 2 hours of a positive appointment experience — before the patient’s attention has moved to other things. Automated review request systems (via text or email through platforms like Weave or Birdeye) sent at this timing consistently generate 3–5× more reviews than unstructured asks. The message should be brief and direct: “Thanks for coming in today, [Name]. If you have 60 seconds, we’d really appreciate a Google review — it helps other patients find us.” Include a direct link; friction at any point dramatically reduces completion rates.
For the full strategic framework connecting patient satisfaction to practice growth, see our guide to patient retention strategies for dental practices. For how visual communication enhances patient understanding during appointments, see our guide to visual aids for dental patient education.
Last Updated: March 2026
For related reading, see our guide on how the patient experience during the consultation drives case acceptance rates.
Sources
- American Dental Association. Patient Experience and Satisfaction Survey. ADA, 2023.
- Armfield, J.M. & Heaton, L.J. “Management of fear and anxiety in the dental clinic: a review.” Australian Dental Journal, 2013.
For more resources on this topic, see our complete guide to patient trust and experience.



